By Alexander Casendino
United States of Incarceration
“It’s a level of suffering that is unprecedented. The degree of suffering and the degree of harm to these patients is really the result of a system that is extremely, extremely broken.”
No, the description above is not of a CIA black site or a sinister underground research facility. The description matches an institution far closer to home: the American prison system and its administration of healthcare to the nearly 2.3 million incarcerated individuals in the U.S.
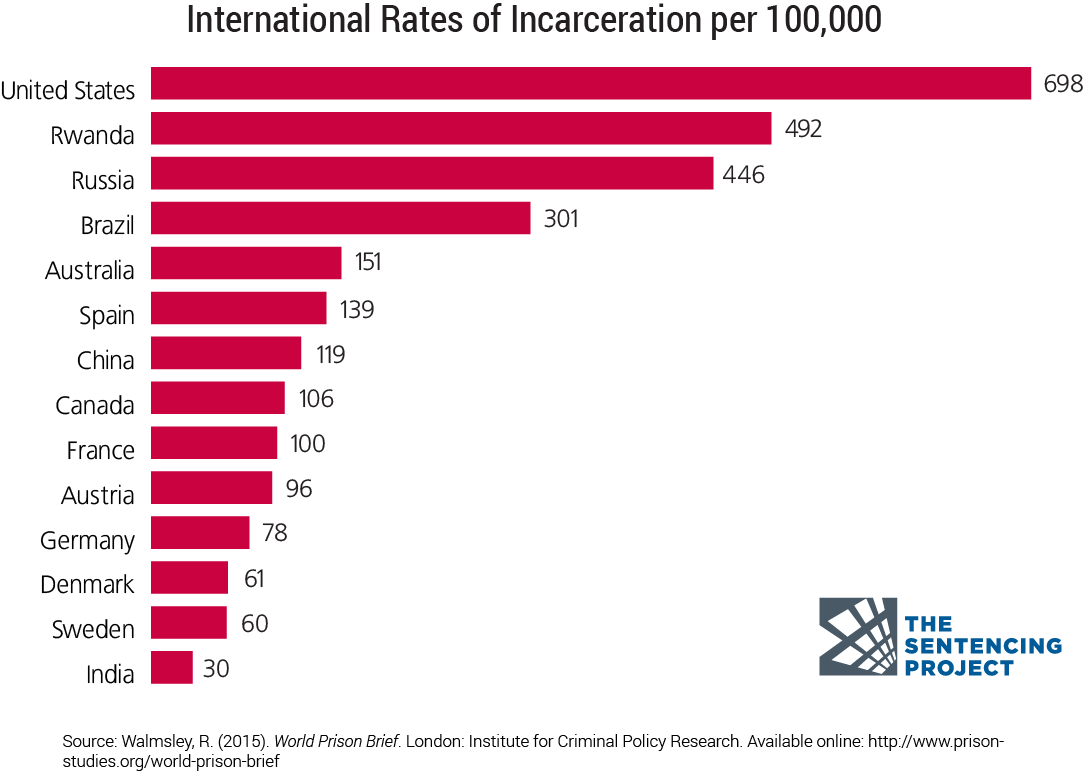
The observation noted above by Alexander Soler, an executive director of the American Civil Liberties Union in Arizona, of the lackluster state of healthcare in U.S. prisons, is deeply intertwined with the explosion of the U.S. prison population. According to the London Institute for Criminal Policy Research, the prison population of the United States has quadrupled in the past 25 years, and the U.S. tops the globe in incarceration rates.
 The financial stress placed upon the rapidly expanding U.S. prison system incentivized local, state and federal prisons to adopt a policy that has led to sinister reverberations in all levels of the prison system: the privatization of health care.
The financial stress placed upon the rapidly expanding U.S. prison system incentivized local, state and federal prisons to adopt a policy that has led to sinister reverberations in all levels of the prison system: the privatization of health care.
Healthcare Hindered
According to the Bureau of Justice Statistics, states spend about eight billion dollars annually on prison healthcare. In an effort to cut costs, more prisons are outsourcing healthcare to for-profit companies such as Corizon Health, the largest private prison healthcare provider in the country, and Correctional Medical Group Companies (CMGC).
Dr. Marc Stern, an expert on correctional health at the University of Washington and former head doctor of all Washington state prisons, estimates that more than half of all state and local prisons and jails have outsourced their healthcare. Additionally, according to a report issued by the Office of the Inspector General in June 2016, federal prison spending on outsourced healthcare increased by 24% to $327 million between 2010 and 2014. Private healthcare providers have aimed to reduce costs when operating within prison facilities and argue that prisoners are receiving adequate medical attention while saving taxpayer dollars in the process. Cost-cutting practices, however, have not mixed well with a prison population that is increasingly in need of greater medical care and services.
After analyzing data collected from surveys of US inmates in local, state, and federal correctional facilities, physicians at the Cambridge Health Alliance and Harvard Medical School uncovered a startling fact: the number of serious medical conditions among convicts were far higher than expected compared to the average American population.
In the official paper published in the American Journal of Public Health in April 2009, the researchers revealed that roughly 40% of inmates of the entire prison and jail population reported a chronic medical condition. The same report unearthed that among inmates with a persistent medical problem, 13.9% of federal inmates, 20.1% of state inmates, and 68.4% of local jail inmates had received no medical examination since incarceration. Infectious disease, mental illness and addiction are common problems for inmates. Unfortunately, the lack of available checkups and services for inmates has resulted in avoidable injury, and in the worst of cases, death. Furthermore, the risks to inmates’ health have been compounded by the reduced coverage provided by private healthcare companies.
History of Neglect
In the 1976 case of Estelle v. Gambelle, the Supreme Court established that ignoring a prisoner’s serious medical needs constitutes cruel and unusual punishment in violation of the 8th Amendment of the U.S. Constitution. After four decades of rising incarceration rates, the precedent of this pivotal case has been repeatedly neglected by private healthcare entities operating within prisons.
From 1975 to 2015, the U.S. prison population quadrupled. Interestingly, Steven Raphael of the University of California, Berkeley, and Michael A. Stoll of the University of California, Los Angeles discovered what drove up the imprisonment rates during this time was not just crime, but policy. Harsh sentencing was believed to deter future crime, and by 2015 all 50 states had adopted mandatory sentencing laws, vastly increasing the number of incarcerated convicts. The growth of the prison population placed stress upon the healthcare providers, who were struggling to catch up with the exponentially growing number of clients in prison.
In February 2015, the private healthcare provider Corizon paid out $8.3m to the family of Martin Harrison, who died two days after being jailed in Alameda County. Harrison was suffering from severe alcohol withdrawal and was allegedly beaten by prison guards, and his family’s lawyers argued that Corizon had failed to provide reasonable care to Harrison. Harrison’s story is not unique: according to an analysis by the financial research firm PrivCo, Corizon has been sued more than 1,300 times, ranging from wrongful death lawsuits to sexual misconduct charges. However, lawsuits have not halted Corizon’s profitability: according to PrivCo, the company’s revenue has grown by 15.6% from 2012 to 2015, amounting to $1.55 billion in net worth.
Path to Reform
Privatization within the U.S. prison system has led to a pattern of irresponsibility and setbacks for criminal justice reform. Just three months ago, the Department of Justice released a statement supporting an end to federal private prisons, citing unsafe conditions within private prisons and lack of adequate security. Federal private prisons provided private healthcare to convicts, resulting in reduced quality of care. While federal private prisons will soon be transferred to government regulation, millions of convicts in public prisons and privately-run state facilities must still rely upon private healthcare providers that routinely fail to protect inmates’ health.
There is a comprehensive set of solutions to pursue in order to initiate greater reform and ensure humane treatment of prisoners. Greater funding for rehabilitation programs, from substance abuse to mental health reform, can target specific prisoner groups and address chronic illnesses. Additionally, greater oversight of private health care providers will ensure that profit is considered a second priority to convicts’ health. Ultimately, Americans on both sides of the prison gate will reap greater rewards, including saved taxpayer dollars and improved health conditions for convicts, by addressing the injustices brought about by the privatization of health care in prison.
Featured Image Source: European Monitoring Centre for Drugs and Drug Addiction






One Comment